I noticed a commentary published in Modern Healthcare (2019) by Ann Marie Benedicto, the vice president of the Joint Commission Center for Transforming Healthcare. She writes that the center found in a recent survey that nearly eight of 10 healthcare professionals cited a lack of leadership (77 percent) and absence of organizational investment (79 percent) as barriers to excellence in patient safety.
A news release issued by the center (2019) shed further light on the survey’s findings, saying that nearly nine of 10 (88 percent) believe inadequate staffing is the biggest barrier to excellence while more than half (54%) believe addressing nurse-patient ratios will improve patient safety.
“Addressing these systemic issues won’t take a tweak here and a new checklist there,” Benedicto writes. “It will take wholesale change and a commitment to adopting and training workers on high-reliability healthcare principles, putting data-driven tools to work—and cultivating a safety culture to sustain these practices.”
The center has long emphasized the importance of data gathering toward finding solutions meeting a health care organization’s unique circumstances and challenges. The point of view expressed by Benedicto and the center is consistent with my experience as a hospital administrator and now an executive with a health care technology company. Too many health care organizations have been slow to invest in the data-gathering tools now available to improve patient safety.
Improving workflow can help mitigate staffing shortages
A particularly overlooked aspect of patient safety is the importance of effective workflow. As Benedicto states in her commentary, about 1 out of 31 hospital patients has a healthcare-associated infection on any given day and as many as a million patients fall in U.S. hospitals. Both infections and falls can be reduced by improved workflow that makes the most important moments in health care more effective – the face-to-face moments when patients and caregivers interact. The communication that occurs during these interfaces have the greatest bearing on the quality, safety and effectiveness of health care.

Studies have documented that both doctors and nurses spend more time interacting with technology than with patients (Higgens, 2017; Tai-Seale, 2017). Vitalacy’s Patient Safety Platform gives health care organizations a way to gather data on the locations and movements of their care providers through the use of Bluetooth-enabled sensors. Working together in collaboration, unit managers and their team members gain insights into where they are working and for how long – the first step toward adjusting workflow and improving performance on preventive interventions such as hand hygiene compliance, which has been shown to have a direct impact on reducing healthcare-acquired infections (HAIs) (Vitalacy, 2019). Better workflow and purposeful rounding also can help to prevent healthcare-acquired conditions (HACs) such as falls, pressure ulcers, venous thromboembolism (VTE), and mistakes relating to nurse fatigue.
In my discussions with health care leaders, I have been emphasizing the importance of developing a real understanding of how their care providers go about their jobs each day. Because workflow varies from hospital to hospital, from unit to unit, a one-size-fits-all approach won’t work. What will work is caregivers developing an awareness of how their everyday actions and routines can prevent HAIs and HACs.
Care providers want to improve patient safety but look to leaders for support and commitment
Developing collaborative work groups is an important aspect of the approach Vitalacy takes with its hospital clients. The success of our approach is ultimately driven by the buy-in and enthusiasm it generates among front-line health care workers. We find that once they understand that our platform makes their unit safer for patients, they buy into the program wholeheartedly.
The caregivers at our client’s medical centers have provided feedback and ideas that have helped us to evolve and enhance our platform. Noting that the Vitalacy system can track the movement of caregivers through their workday, one care provider asked if the system could track when and for how long caregivers interacted in patient rooms. Her question rose from a concern about the high fall rate at the medical center due to severely immuno- compromised end-stage cancer patients at high risk for falls and other complications.
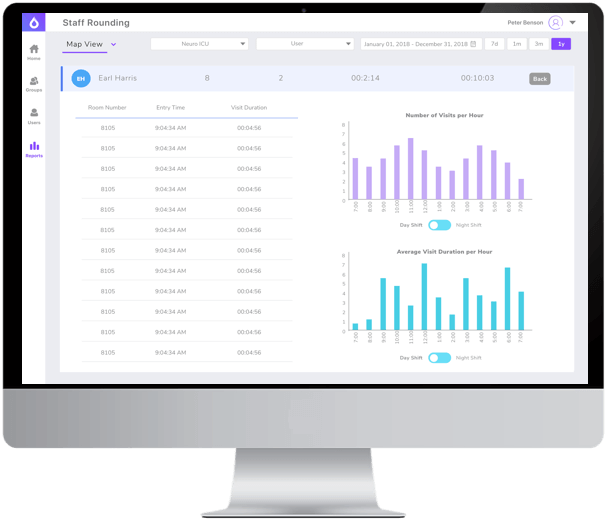
This question led to the development of Vitalacy’s purposeful nurse rounding data module, which was implemented for the first time at this medical center. The module identifies which staff member completed rounding in each room, at what time, and for how long. By viewing activity by staff and room, managers can ensure that patients get alerts when patients have not been visited when necessary and can identify high- and low-performing staff to target education and training. The timing and frequency of visits can be set for patients and adjusted to alert for higher-risk patients.
The Joint Commission Center for Transforming Healthcare’s survey shined a light on the desire of care providers to improve patient safety while noting that many of these caregivers feel that they alone cannot make enough of an impact to help an organization achieve zero harm. It’s up to hospital leadership to make high reliability a crusade across all levels of an organization and to gain the confidence of their workers that together they are truly making strides toward zero harm.
Request a demo of Vitalacy’s Automated Hand Hygiene Monitoring Solution today!
References
Benedicto, AM. Commentary: Healthcare remains unprepared for today’s complex challenges. Modern Healthcare, Aug. 31, 2019.
Higgens, L, et al. Hospital nurses’ activity in a technology-rich environment. Journal of Nursing Care Quality, July/Sept. 2017, 32(3):208-217.
Tai-Seale, M, et al. Electronic medical record logs indicate that physicians split time evenly between seeing patients and desktop medicine. Health Affairs, April 2017, 36(4).
The Joint Commission Center for Transforming Healthcare news release. Survey: Healthcare Survey: Nearly 2 Million Health Care Professionals Don’t Feel They Have Tools, Training to Safely Care for Patients, Aug. 22, 2019.
Vitalacy, Inc. Finding new ways to prevent healthcare-acquired infections and conditions. Mar. 14, 2019.
Author
-

Vitalacy is committed to reducing patient harm in healthcare through better hand hygiene and patient safety solutions. Bluetooth-enabled smart sensors and wearables help improve outcomes and Leapfrog Hospital Safety Grades.



