It’s well known among infection control experts that hand hygiene is the best defense against the spread of viral and bacterial infections. Soap and water lifts and washes different kinds of bacteria and viruses – including the various strains of coronavirus – down the drain. In addition to using soap and water, healthcare providers should incorporate an alcohol-based hand sanitizer into their hand washing routine because it is more effective against certain kinds of germs (CDC, 2017).
As the coronavirus (COVID19) infects more people around the world each day, media stories have begun to advise readers and viewers about the importance of frequent hand washing. While images of individuals wearing masks often accompany headlines, photographs of hand washing would be more helpful.
When I heard that the coronavirus was spreading to the United States, one of the first things I did was tell my family to get in the habit of frequent hand washing, not only to prevent a possible coronavirus infection, but to prevent the flu, the common cold and other kinds of viral and bacterial infections.
These kinds of gentle reminders do prevent infections and save lives, and they will continue to do so. We never fully see what we’re able to prevent, but Vitalacy has data showing that reminders reduce infections.
Reminders and alerts must be designed with human factors in mind
In the healthcare environment, reminders sometimes come in a variety of ways, often in the form of a beep, ring, ping or text message. Hospital staff members must continually process the various alerts they receive before deciding the most appropriate response. Concern about “alert overload” is well-documented and justified.
As new kinds of technology is deployed within healthcare settings, we must pay special attention to how care providers interact with it. The study of how humans interact with technology and other elements within their work environment is known as “human factors.”
Well-aware of the challenges facing front-line healthcare workers, Vitalacy designed its hand hygiene and workflow monitoring technology with human factors in mind.

To remind care providers of hand hygiene compliance at the point of care, Vitalacy devised a private, tactile reminder – a brief vibration – that is felt only by the care provider. This subtle reminder provides instantaneous feedback in real time and has proved to be effective in increasing hand hygiene compliance (Vitalacy, 2019). The vibration improves mindfulness about hand hygiene.
Well-designed reminders give providers a choice
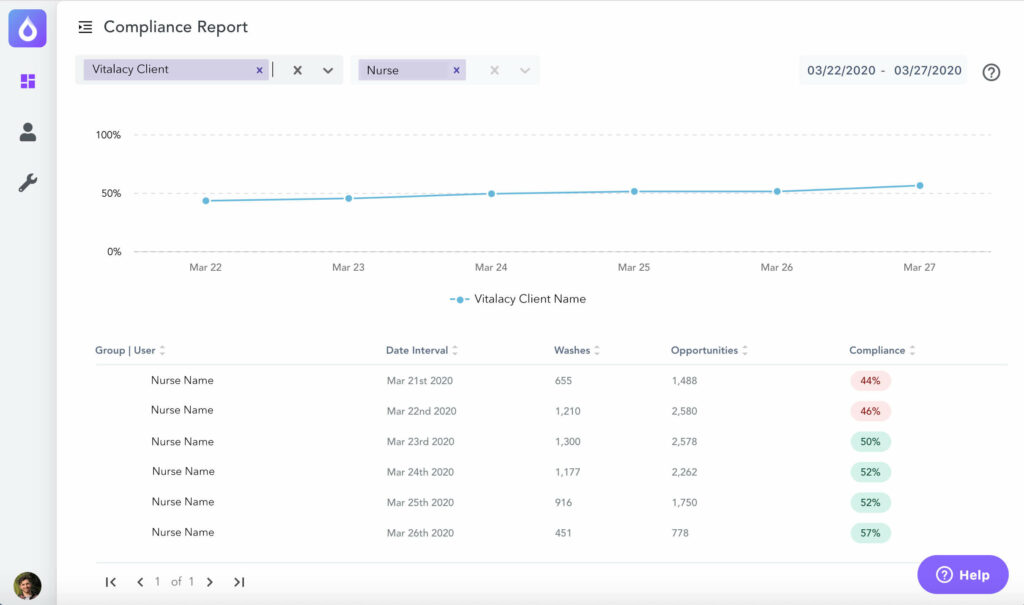
During a recent implementation at an academic medical center, Vitalacy’s hand hygiene compliance tracking found that compliance was about 30 percent when care providers did not receive vibration alerts on their wristbands. After activating the wristband alerts, the compliance rate increased to more than 70 percent over the course of about one week (Vitalacy, 2019).
These real-time compliance data provided evidence that the vibration alerts made patient care safer. In addition, the built-in, optional vibration alert feature gives providers the power to choose whether to use the vibration alerts rather than having a product engineer make that decision for them.
Vitalacy’s technology emphasizes the safety culture tenet of using personal performance data gained from monitoring to drive improvement rather than to assign blame. Capable of creating compliance reports by individual, unit and organization, the technology enables each caregiver to feel personal engagement and responsibility for the success of the overall initiative. This feature also creates fun competitions between individuals and units for the best compliance scores – all in the name of patient safety.
It’s important to empower care providers with personal responsibility
In writing about electronic hand hygiene monitoring systems, Son et al., (2011) raised the importance of empowering healthcare providers within a group or unit with “the responsibility to identify their own obstacles and barriers to proper hand hygiene, create action plans to remove them, and establish their own goals that can lead to sustainable improvement over time. . . (These systems) allow for tracking and reporting on an individual healthcare worker’s performance, so they can receive personal feedback . . . Most importantly, electronic monitoring systems tell the truth, better enable accountability, and can drive real performance improvement from an honest baseline. Accurate, reliable, timely, and actionable data is the key benefit.”
Yes, gentle reminders help, whether they’re to your family members about the coronavirus or to hospital care providers about hand hygiene and other aspects of infection control. The key is to do them in a way that empowers care providers rather than causing fear and disruption. Done right, reminders can provide constant reinforcement for doing the right things at the point of care while creating the kind of personal engagement required to improve patient safety at your hospital.
Request a demo of Vitalacy’s Automated Hand Hygiene Monitoring Solution today!
References
Centers for Disease Control and Prevention. Clean hands count for safe healthcare, May 5, 2017.
Son C, et al: Practically speaking: Rethinking hand hygiene improvement programs in healthcare settings. American Journal of Infection Control, 2011;39(9):716-724.
Vitalacy, Inc. Finding new ways to prevent healthcare-acquired infections and conditions. Mar. 14, 2019.
Author
-

Vitalacy is committed to reducing patient harm in healthcare through better hand hygiene and patient safety solutions. Bluetooth-enabled smart sensors and wearables help improve outcomes and Leapfrog Hospital Safety Grades.



