A recent study published in Infection Control and Hospital Epidemiology takes a close look at how antibiotic stewardship programs have fared against Clostridioides difficile (C. diff) infections (Vaughan, et al., 2019). The 500,000 C. diff infections occurring in the United States annually lead to about 15,000 deaths.
The Joint Commission made having an antibiotic stewardship program a condition of hospital accreditation in 2017 and expanded the requirement to ambulatory care centers in 2019. The Centers for Disease Control and Prevention (CDC) recommends that antibiotic stewardship programs at critical access hospitals with more than 25 beds include a pharmacist and a physician leader.
The Vaughan study found that the effectiveness of antibiotic stewardship programs has been uneven, especially in smaller hospitals, where access to infectious disease expertise and deploying diagnostic stewardship strategies can be challenging. Larger hospitals were more likely to meet both The Joint Commission’s and CDC’s recommendations.
The Vitalacy team gave some thought into how electronic hand hygiene monitoring can help hospitals to make antibiotic stewardship more effective.
1. Electronic hand hygiene monitoring can track the use of both soap and hand sanitizer dispensers
According to CDC guidelines, C. diff infections are best prevented by hand hygiene using soap and water rather than hand sanitizers. C. diff organisms have hard shells protecting them from alcohol; the best way to remove them is to wash them down the drain. Soap and water are also more effective against the flu virus and the norovirus.
According to another recent study (Pidot, et al., 2018), infections caused by E. faecium are increasing due to this bacterium’s tolerance to alcohol used as a killing agent. The study tested the alcohol tolerance of 139 hospital isotopes of E. faecium obtained between 1997 and 2015. E. faecium is a species of enterococcus, which causes 10 percent of the world’s hospital-acquired infections. In the U.S., this bacterium is a leading cause of sepsis, a deadly blood infection.
The study shows that bacteria can develop resistance not only to antibiotic medicines per se, but to other substances, such as alcohol, as well. These findings provide more evidence of how bacterial adaptation is complicating hospital infection control.

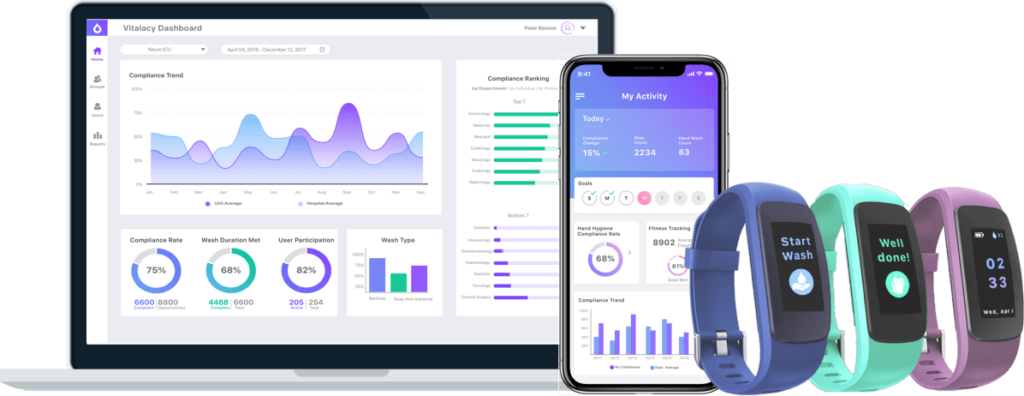
Vitalacy’s electronic hand hygiene monitoring technology tracks the use of both soap and hand sanitizer dispensers. The dispenser sensors track exactly how often and for how long the dispensers are used and how much soap or sanitizer is dispensed. The technology not only helps hospitals to improve their overall hand hygiene compliance, it helps to reinforce the importance of making both soap and hand sanitizer a part of the daily hand hygiene regimen.
2. Electronic monitoring improves hand hygiene compliance
While tracking the use of dispensers, the Vitalacy system also provides hand hygiene reminders to care providers throughout a shift. The reminders come in the form of a gentle vibration at each hand hygiene opportunity to a wristband worn by each provider. Each wristband has a Bluetooth connection to strategically positioned dispenser sensor tags that track every patient room entry and exit along with wash frequencies.
Providing real-time reminders at the point of service is a pivotal step in increasing and sustaining hand hygiene compliance and patient safety. The dispenser sensors and wristbands work together at the point of care to remind caregivers and drive up compliance rates.
The ability to track the quality of each hand wash is a primary differentiator of the Vitalacy system. The sensors within the wristband monitor subtle hand movements while care providers wash their hands; these observational data are fed into a patented algorithm that in turn enables the wristband to provide feedback to its wearer on how to improve hand-washing technique.
The Vitalacy system tracks individual, unit and organizational hand hygiene performance. Location beacons installed in patient rooms monitor hand hygiene opportunities, and a gateway sends all the data to a cloud database. A reporting system accessible via a mobile app and the web shows how often, how long, and how well individuals are washing their hands and provides feedback and reminders about hand hygiene.
3. Electronic hand hygiene compliance monitoring can reduce infections and antibiotics use
Good hand hygiene stops the spread of all healthcare-associated infections, including those that may need to be treated with antibiotics. Less infections means less antibiotics used to treat them.
Both Vitalacy’s experience and various studies have shown the correlation between hand hygiene compliance and reduced infections. In early 2017, the Vitalacy system was implemented in about half the medical and surgical beds in an academic medical center with a higher-than-average rate of healthcare-associated infections.
Immediately after implementation, Vitalacy’s automated hand hygiene compliance tracking found that the hand hygiene compliance rate was only about 20 percent when health care providers did not receive vibration alerts on their wristbands. After turning on the wristband alerts, the compliance rate increased to more than 60 percent over the course of two days.
The medical center was eventually able to increase compliance to more than 70 percent based on 225,000 observations per quarter. Infection incidence decreased both on the monitored units and medical center-wide for two consecutive quarters. Due to these initial results, the medical center is expanding the project to all patient care units (Vitalacy, 2019).
The results of various other studies have been promising. Michael et al. (2017) reports that an automated system with immediate feedback caused a rapid and sustained improvement in compliance. For example, one unit improved from 54 percent compliance over 12 months based on 88 direct observations to 98 percent compliance over 12 weeks based on 140,000 automated observations.
Another study of an electronic system shows an increase of hand hygiene compliance of 25.5 percent, a decrease of healthcare-associated MRSA infections of 42 percent from baseline, and a savings of $434,000 over the study timeframe (Kelly et al., 2016). “Across the entire hospital, periods of improved hand hygiene compliance led to lower infection rates,” the authors state. “We believe the monitoring system aided nursing leadership’s ability to drive change and improve staff performance, by providing real-time reliable (compliance) data.”
Request a demo of Vitalacy’s Automated Hand Hygiene Monitoring Solution today!
References
Kelly JW, et al: Electronic hand hygiene monitoring as a tool for reducing healthcare- associated methicillin-resistant Staphylococcus aureus infection. American Journal of Infection Control, 2016;44:956–957.
Michael H, et al: Durable improvement in hand hygiene compliance following implementation of an automated observation system with visual feedback. American Journal of Infection Control, 2017;45:311-313.
Pidot, et al. Increasing tolerance of hospital Enterococcus faecium to hand wash alcohols. Science Translational Medicine, August 1, 2018.
Vaughan VM, et al. Antibiotic stewardship teams and Clostridioides difficile practices in United States hospitals: A national survey in The Joint Commission antibiotic stewardship standard era. Infection Control & Hospital Epidemiology, Feb. 2020;41(2):143-148.
Vitalacy, Inc. Finding new ways to prevent healthcare-acquired infections and conditions. 2019.
###
Author
-

Janel Nour-Omid was inspired to start Vitalacy after losing her grandfather to a Healthcare-Acquired Infection. Through her background in computer science and product development and deep fascination in human behavior, she launched the Vitalacy platform designed to protect caregivers and patients from preventable infections and conditions. She was recognized in Forbes 30 Under 30 in Healthcare in 2020.



