Health care is fast – and stressful. It’s no wonder why so many nurses suffer from various kinds of fatigue or trauma. And, unfortunately, due to the speed and pressures of providing health care, nurses rarely have opportunities to talk to their managers and colleagues about their wellbeing.
The nurse fatigue and trauma statistics are stunning but of no surprise to clinicians working on the front lines of health care.

Psychological and physical stressors contribute to nurse fatigue. Working long hours, especially on one’s feet, can contribute to nurse fatigue, and other stressors affecting the work environment or culture cannot be discounted. These stressors can include time pressure, lack of leadership support, exposure to work-related violence or threats, and exposure to illness or injury.
Virtually every nurse experiences secondary trauma, which is caused by witnessing an unsettling event that adversely affects another human being. These events can include the death of a patient, a serious injury to a child, or an act of violence. This form of trauma is also known as compassion fatigue.
Another trauma-related disorder common among nurses is post-traumatic stress disorder (PTSD). As many as one in four nurses experience PTSD at some point during their careers, Emilie Le Beau Lucchesi reported for the New York Times (2019). In some settings, the risk may be higher than in others. A recent study published in the Journal of Heart and Lung Transplantation found a range of 17 percent to 48 percent of intensive care nurse groups experiencing PTSD; the condition led to 14 percent of the nurses resigning and one suicide attempt (Sanchez M, et al., 2019).
PTSD can stem from experiencing a distressing event first- or second-hand, or even from repeatedly hearing details about a fatal, violent or harmful occurrence. PTSD produces unwanted memories, flashbacks, nightmares and other reactions when those suffering from the disorder are reminded of the event.
Fatigue and trauma continue to contribute to high nurse turnover. According to the Nursing Solutions Inc. 2019 National Health Care Retention and RN Staffing Report, the turnover rate for bedside RNs is 17.2 percent per year and the average cost to replace a bedside registered nurse is estimated at more than $50,000. The average hospital loses $4.4 million to $6.9 million each year due to turnover (NSI, 2019). Nurses providing direct patient care in hospitals tend to have the highest burnout rates.
Hospitals leaders are making nurse wellbeing a higher priority
Hospital leaders are making nurse wellbeing a higher priority because research shows a correlation between care provider satisfaction, provider engagement, and better quality and safety results (Ratanjee & Drenkard, 2019). Higher nurse engagement is statistically related to less patient complications, lower mortality indexes, and 41 percent fewer patient safety incidents. This research also shows that hospitals with the least engaged nurses pay $1.1 million per year in malpractice claims than do hospitals with highly engaged nurses.
For example, Banner Health began a program for nurses that offers guided imagery or another healing therapy option called Reiki for about 15 minutes per session. This involves having each nurse listen to an audio presentation that helps them to visualize and relax. The program measures the nurses’ discomfort on a one-to-10 scale at the start of the process, and nurses are often able to reduce their stress or fatigue as a result of the program (Gallese, 2019).
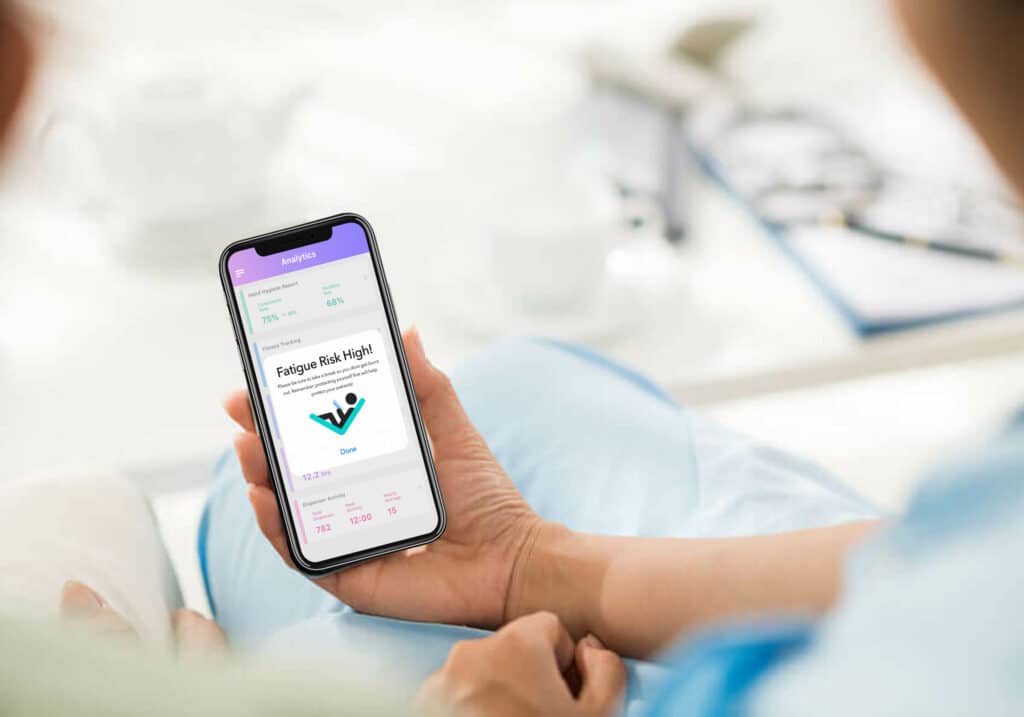
Vitalacy’s nurse fatigue scoring tool notifies nursing unit managers when a nurse is experiencing symptoms of burnout caused by factors such as long shift duration, high shift frequency and miles traveled. These indicators often prompt conversations between nurses and their managers about physical and emotional stressors they may be experiencing.
Lending a kind ear and showing concern are important steps toward building better satisfaction and engagement among nurses. Having support systems in place to assist nurses in need can help even more. In work groups with its clients, the Vitalacy team explores with them how nurse fatigue data can lead to important conversations about patient safety and nurse wellbeing.
Healthcare is fast – and stressful. By allowing nurses opportunities to slow down and express their feelings, hospital leaders can make patient care more rewarding and satisfying for nurses and more effective for patients.
Request a demo of Vitalacy’s Automated Hand Hygiene Monitoring Solution today!
References
Gallese P. Helping caregivers manage stress, burnout and fatigue: an interview with Linda Bennet, Ph.D., Vitalacy Blog, July 30, 2019.
Le Beau Lucchesi, E. For nurses, trauma can come with the job. The New York Times, May 7, 2019.
Nursing Solutions Inc. (NSI). 2019 National Heath Care Retention and RN Staffing Report. 2019.
Ratanjee V & Drenkard K. 3 strategies hospital leaders can use to get rounding right. Gallup Workplace, Nov. 11, 2019.
Sanchez M, et al. PTSD in Tx ICU nurses. The Journal of Heart and Lung Transplantation, April 2019;38(4):S93-S94.
Author
-

Vitalacy is committed to reducing patient harm in healthcare through better hand hygiene and patient safety solutions. Bluetooth-enabled smart sensors and wearables help improve outcomes and Leapfrog Hospital Safety Grades.



